By Marni Jameson
Orlando Sentinel.
Like many working moms, Hope Bott of Orlando usually put her family’s health needs ahead of her own, said the wife and mother of three boys.
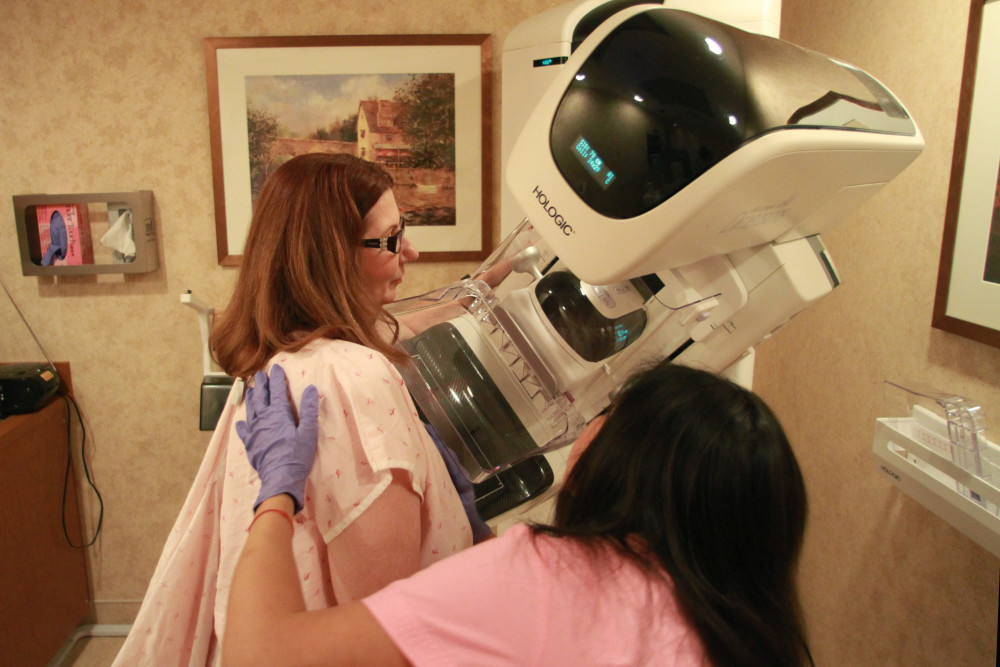
So when a mobile-mammography bus pulled up to her workplace in March, she got on board.
Bott, 38, an operations analyst for Pepsi, has a family history of breast cancer, so she wanted to get tested.
Five days after her screening, she got a letter recommending more testing.
She was referred to a Florida Hospital doctor, who ordered another mammogram, an ultrasound, an MRI and, ultimately, a biopsy.
Three anxiety-ridden weeks later, Bott got her results. “Thankfully, it was benign,” she said.
Although she didn’t enjoy the worrying, she’s grateful she had the testing
Bott became part of the health-care trend toward meeting patients where they are.
Throughout Central Florida, more mobile health-screening services are rolling to businesses and community centers, where health professionals check patients for breast cancer, heart problems, stroke risk and more.
Those behind the programs say they save lives and improve access.
But some health analysts argue that all that screening really isn’t necessary and that the vehicles are a way for hospitals to troll for patients, boost physician referrals and sell unneeded diagnostic services.
The mobile services offer accessibility and convenience, which more patients want, said Marla Silliman, senior vice president of women’s services at Florida Hospital, where she oversees a women’s health bus that offers mammography, heart screenings and bone-density testing.
“Employers like the mobile services because they want to provide preventive services to employees without a lot of downtime,” Silliman said.
A preliminary review of nonprofit hospitals’ tax records, which reflect their spending, has shown that the number of hospitals investing in mobile-screening vehicles nationwide has increased dramatically in recent years, said Gerard Anderson, professor of health economics at the Johns Hopkins Bloomberg School of Public Health.
In Central Florida, mobile services are clearly trending up.
The Florida Hospital for Women Health Coach has screened 7,000 patients since the service started in 2011.
It is on track to see 6,000 patients this year alone, and Silliman hopes the bus will eventually screen 8,000 a year.
Many of the women who used Florida Hospital’s bus service would never have been screened if it hadn’t come to them, Silliman said.
Seventy percent had never had a mammogram.
“We don’t have a shortage of mammography centers in Central Florida, but women aren’t accessing them,” she said.
Making mobile mammography available to women who were not getting mammograms is a benefit, Anderson said, but there’s a benefit for hospitals, too.
“The hospitals make some money from the screenings, but the real money comes from the additional testing and procedures that result,” said Anderson. “A lot of these screenings result in false positives and put women through unnecessary and potentially dangerous testing.”
The collateral damage is what people overlook, said Dr. Otis Brawley, chief medical officer of the American Cancer Society, referring to the invasive testing, additional radiation and unnecessary treatments that can result from screenings.
“You have to involve many people and harm some to help one,” said Brawley, an oncologist and author of “How We Do Harm: A Doctor Breaks Ranks About Being Sick in America.”
Brian Klepper, chief executive for the National Business Coalition on Health, a Washington-based organization that represents 4,000 U.S. businesses, calls the rapid growth in mobile medicine “opportunistic.”
“While outreach mobile services may seem attractive,” said Klepper, “often their design is to be referral buses to drive more patients into the mother ship, where they go in for much more expensive care and become fodder for financial return.”
Silliman strongly disagrees.
“This model was not built as a feed strategy,” she said. “It is purely for community outreach. We intentionally take care of a percent of patients who do not have insurance.
It’s also OK if a patient needs follow-up and doesn’t want to come to Florida Hospital. Does it have a downstream benefit for us? Yes. But we’re not banking on that as the main reason to do it.”
Florida Hospital’s bus is on the road five days a week.
Four days it rolls to businesses, churches or schools, where patients are likely to have insurance. However, one day a week, the bus targets underserved communities, Silliman said.
The Florida Hospital bus is one of a handful of mobile-mammography units in the area.
The Women’s Center for Radiology, in Orlando, has been offering mobile mammography for about 25 years, said center Director Vicki Belmont, who has also witnessed the recent boom in the field.
Beyond mammography, Life Line Screening, a national company that started in Florida, conducts more than 1 million mobile screenings a year nationwide for more than 20 health conditions at 16,000 events, said spokeswoman Joelle Reizes.
Of the 7,000 women the Florida Hospital bus has screened, one in four was uninsured, said Jennifer Robertson, a spokeswoman for Florida Hospital.
More than 800, including Bott, were referred to a physician for follow-up testing or treatment. Twelve women, or 1.5 percent, were diagnosed with either breast cancer or a cardiac ailment.
“For me, having a mobile unit come to where I work was a potential lifesaver,” said Bott. “If it hadn’t come, I don’t think I would have gone for a mammogram.”
That’s proof for Silliman that the concept is working.
“If one coach can screen 8,000 women a year, and we grow to five coaches, we could see 40,000 women a year,” she said.
To screen or not to screen
When a mobile-mammography service rolls up to a workplace or community center, women need to ask whether the screening is appropriate for them, experts say.
That’s not as easy as it sounds.
Controversy still surrounds the question of which women should receive screening mammograms and when.
The American Cancer Society recommends yearly mammograms starting at age 40 for women who have no family history of breast cancer.
However, the U.S. Preventive Services Task Force, a group of independent health experts convened by the U.S. Department of Health and Human Services, says routine screening for average-risk women shouldn’t begin until age 50, after which they should have a mammogram every two years.
Marla Silliman, who heads women’s health services at Florida Hospital, favors the society’s guidelines and adds that her service won’t screen any woman who has had a mammogram within the past year, which coincides with what most insurance plans will cover.
But Gerard Anderson, professor of health economics at the Johns Hopkins Bloomberg School of Public Health, said he “would tend to use the USPTF guidelines, which are more objective.”
Over-testing is a concern not only because it’s costly but because more invasive follow-up procedures can do harm. Mammograms emit small amounts of radiation.
Studies have found that having many mammograms during a lifetime appears to contribute to breast cancer, though the risk from such exposures is low, experts say.